Lumbar Spine Disc Injury Rehab | Week 01

PROGRAM STAGE PRE-REQUISITESTo enter this program you must:
1) Have a confirmed diagnosis of a lumbar spine disc bulge and/or herniation via an MRI or CT imaging scan (Xray alone is not sufficient); 2) Have seen a Physiotherapist or medical practitioner for a assessment of your back injury and clearance to start a mobility and rehab program; 3) Have no additional complications to the disc injury such as a fracture or spondylolithesis; 4) Have no unremitting/constant pain or neural symptoms below the knee, combined with a lateral spinal shift; 5) NOT have a diagnosis of unresolving nerve root entrapment that requires surgical intervention. |
Physio Check-InAs this is the first stage and the first week of the program, it is very important that you 'check in' with a Physiotherapist to assess which exercises are appropriate for you in the first 4 weeks (stage 1). The mobility side glides in standing and/or against the wall found in SET B in the first few weeks that can help people with sciatica and a lateral spinal shift, but only should be done initially under Physio supervision to determine if they are appropriate and they are effective in centralising pain, reducing sciatica / neural leg symptoms and improving the lateral shift.
|
Program InstructionsFor lumbar spine disc injuries, this 'week 1' can start anytime from the acute onset of the injury, to weeks after the original injury and onset of pain. It does not have to be exactly after the initial pain or date of injury. Symptoms can be still present, have become worse of better. It's simply the first week of the rehab phase to start with. Depending on the disc bulge type and severity, some exercises maybe be omitted or continued throughout each week as needed. There are many different presentations of disc pain, and whether your pain is central, one sided, bilateral, you have referred pain, sciatica, altered sensation or a lateral shift, the exercises in the initial weeks of rehab are to centralise the pain, reduce the mechanical derangement and dysfunction and activate the inner core muscles to transition into stage 2 of rehab. Watch the seminar video as well as this week’s videos to help guide you through the process in addition to the program instruction and exercise instruction.
This week, you are aiming to improve lumbar spine extension (backward movement) range of movement (not focusing on flexion) and reduce your back and/or leg referred pain and symptoms, or at least move the pain out of the leg towards the back (centralisation). Your flexion range of movement (forward movement) may improve and be less painful from getting better extension movement, but you are not to repeated flexion to improve the flexion movement in this stage. You may need to focus on lateral movement if you have a lateral shift or pain on one side (as well as referred symptoms in the leg). Most of the time it is more important to move / reduce the referred pain in the leg than to reduce the back pain or get your movement better. DAILY EXERICSES In the first 4 weeks of stage 1 you have 'daily exercises' which you can use as a ritual for morning and night, to help you get moving first thing in the morning, and then again in the afternoon if you stiffen up (or whenever you need during the day or night). The daily exercises are designed to help you loosen up enough to then start the mobility and rehab A and B exercises (see below), as sometimes in the acute stage you are too sore, stiff and have too much muscle spasm to attempt or get the mobility and rehab exercises done. So the daily exercises assist with this. If needed you can to the pelvic tilts and rocks in bed, then move to the floor for the 4 point rocks and the traction. MOBILITY EXERCISES Aim to do the Mobility exercises 3-4 separate sessions per day, EVERY day for the first week. You may need to do one set or 2 sets of each exercise and work the exercises in a 'circuit' rather than do all sets of each exercise in a row. Lying on the floor in a 'crook-lying' supine position resting is better than lying on a sofa, sitting or lying in bed. If the 'rotations knees' is painful to hold, try the controlled rotations exercise instead to loosen up until you can do the sustained version. ‘SET A’ EXERCISES For Set A, these needs to be done 2 x per day, every day. You could do say one round of the exercises in the morning and one round at afternoon or night. These are best done straight after the Mobility exercises as you should be looser at that point. The hip hinge exercise in Set A is not really an exercise, but is there to teach you the way you must move throughout the day should you need to 'bend down' or get items from a lower height, to lift a baby, pick up shopping bags etc. This will keep your spine in neutral and help to stop bending forward at the lower back. SET B EXERCISES For this week, Set B is only needed to be done if able or needed, meaning you have access to a partner for traction or you need to do the side glide exercises if you have a lateral shift or one sided pain. Special NotesAvoid long periods of sitting, and when you can you stand more than you sit throughout the day. Don't do any heavy lifting, avoid squats and deadlifts. The big four things to avoid in the first few weeks are sitting, bending , lifting and squatting. There is a element of rest needed like any injury - but it's rest from aggravating positions, axial load and flexion load, so try to keep moving, walking here and there, but don't attempt any impact exercise, classes, long walks, running or even biking (as you will be in flexion). The cross trainer may be a good form of exercise in week 2 onward depending on your level of recovery. If you are still at work, the use of a stand-up desk is ideal to reduce your time sitting in the day, and help you avoid aggravating the problem from sustained sitting all day.
SPECIAL NOTE: SET B: *Set B exercises - Side glide in standing and against the wall exercises are for only those who have a lateral disc bulge with a shift and one sided pain* For further advice on long term movement habits, spinal load limits, and posture rules once you have recovered, see the special notes section in the Stage 7 post-program stage. |
SPECIFIC EDUCATION VIDEOS FOR THIS WEEK
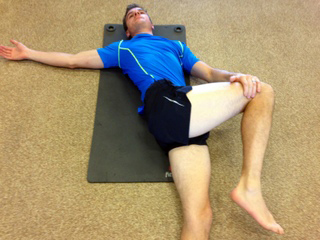
DAILY EXERCISES
| 2-3 |
x / day |
7 |
x / week |






.jpg)
.jpg)
.jpg)

-L.jpg)
-L.jpg)




